 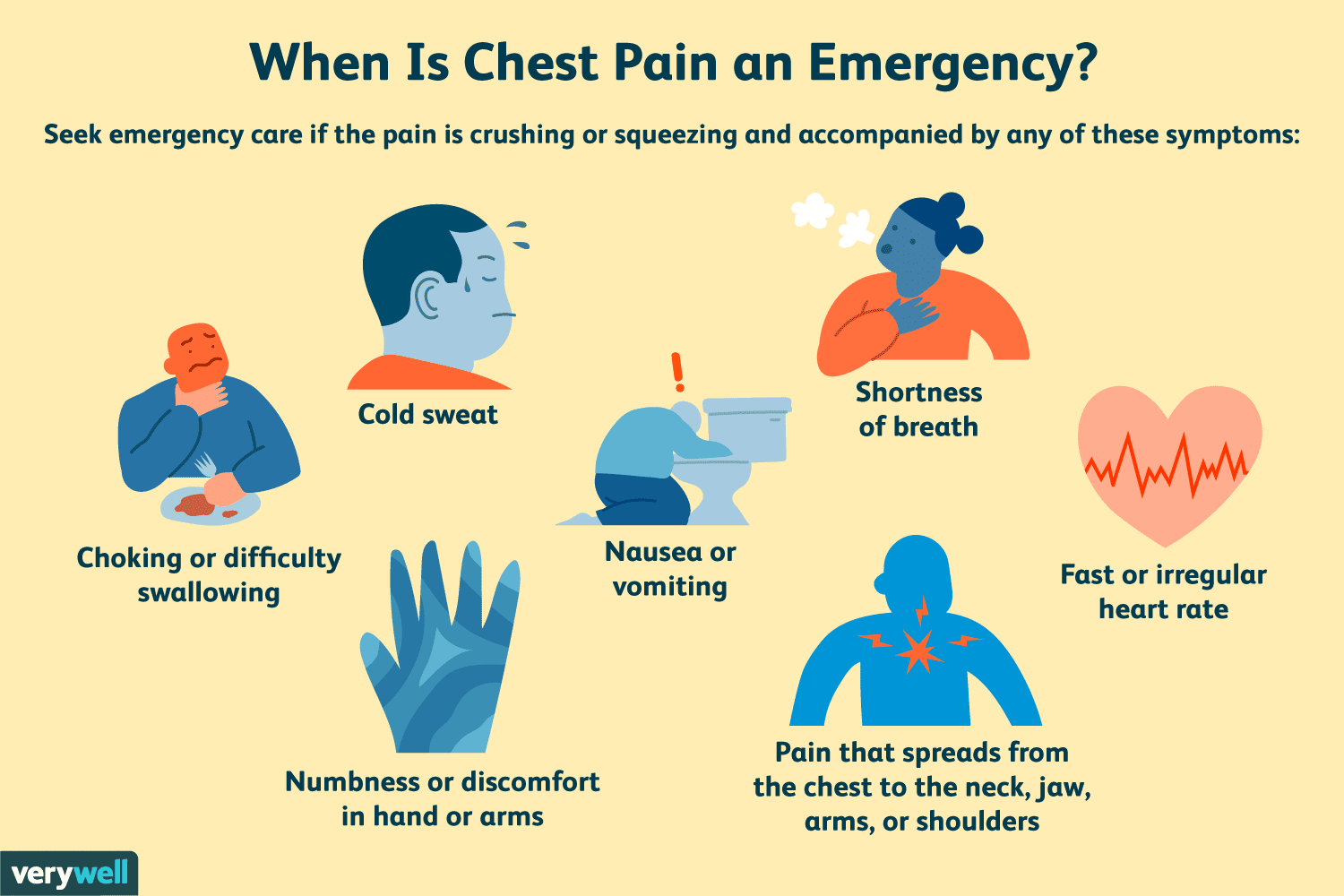
The first decision point for most physicians is to determine whether the patient needs immediate referral to the emergency department for further testing to determine whether the chest pain is an acute coronary syndrome (ACS) caused by coronary ischemia. Panic disorder and anxiety states often cause chest pain and shortness of breath physicians should consider using a single validated screening question to confirm the diagnosis. 31, 32Ĭlinical review and observational studies Gastroesophageal reflux disease should be considered in patients with burning retrosternal pain, acid regurgitation, and a sour or bitter taste in the mouth. Patients with localized musculoskeletal pain that is reproducible by palpation or pain reproducible by palpation of the parasternal costochondral joints likely have chest wall pain or costochondritis. 
Unblinded randomized controlled trials and clinical reviews Patients who have chest pain with a low to intermediate probability of coronary artery disease not requiring immediate referral to the emergency department should be evaluated for coronary artery disease with exercise stress testing, coronary computed tomography angiography, or cardiac magnetic resonance imaging. 21, 22Ĭlinical reviews and consensus expert opinion The presence of ST segment changes, new-onset left bundle branch block, presence of Q waves, and new T-wave inversion increases the likelihood of acute coronary syndrome and acute myocardial infarction these patients should be referred immediately to the emergency department. Twelve-lead electrocardiography should be performed on all patients in whom cardiac ischemia is suspected. 
Smaller clinical trials of validated decision rules Physicians should consider using a validated clinical decision rule such as the INTERCHEST rule or the Marburg Heart Score to stratify risk in patients with chest pain. When patients present to the primary care office with chest pain, physicians should consider age, sex, and type of chest pain to predict the likelihood that it is acute coronary syndrome caused by coronary artery disease. As such, the initial diagnostic approach should always consider a cardiac etiology for the chest pain unless other causes are apparent. 2 Differentiating ischemic from nonischemic causes is often challenging because patients with ischemic chest pain may appear well. 2, 3, 5, 6 No definitive diagnosis may be found in as many as 15% of patients. 2 Other potential factors include pulmonary etiologies (pneumonia, pulmonary embolism ), psychological etiologies (panic disorder), and nonischemic cardiovascular disorders (congestive heart failure, thoracic aortic dissection). 2 – 4 The most common causes of chest pain in the primary care population are chest wall pain (20% to 50%), reflux esophagitis (10% to 20%), and costochondritis (13%). 1 Cardiac disease is the leading cause of death in the United States, yet only 2% to 4% of patients presenting to a primary care office with chest pain will have unstable angina or an acute myocardial infarction. Other less common, but important, diagnostic considerations include acute pericarditis, pneumonia, heart failure, pulmonary embolism, and acute thoracic aortic dissection.Īpproximately 1% of all ambulatory visits in primary care settings are for chest pain. In those with low suspicion for ACS, consider other diagnoses such as chest wall pain or costochondritis, gastroesophageal reflux disease, and panic disorder or anxiety states. 
Those at low or intermediate risk of ACS can undergo exercise stress testing, coronary computed tomography angiography, or cardiac magnetic resonance imaging. Patients with suspicion of ACS or changes on electrocardiography should be transported immediately to the emergency department. Twelve-lead electrocardiography is recommended to look for ST segment changes, new-onset left bundle branch block, presence of Q waves, and new T-wave inversions. The Marburg Heart Score and the INTERCHEST clinical decision rule can also help estimate ACS risk. A combination of age, sex, and type of chest pain can predict the likelihood of coronary artery disease as the cause of chest pain. Initial evaluation is based on determining whether the patient needs to be referred to a higher level of care to rule out acute coronary syndrome (ACS). Approximately 1% of primary care office visits are for chest pain, and 2% to 4% of these patients will have unstable angina or myocardial infarction. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
